Colorectal cancer is a type of cancer that starts in the colon or rectum, both of which are parts of the large intestine. It begins when abnormal cells in the lining of the colon or rectum grow uncontrollably, often first appearing as a polyp.1 While not all polyps become cancerous, some may develop into cancer over time.1,2
Colorectal cancer remains a serious health concern in the United States and around the world. It is the second leading cause of cancer-related death in the United States when numbers for men and women are combined.3 Recent trends show both progress and continued concern, with data indicating that new cases decreased by 0.6% annually in males and increased by 0.3% annually in females.4 Death rates have been decreasing in older adults over the past decades, likely because of increased screening, earlier detection, and improved treatment.1 However, the American Cancer Society reports that death rates among younger adults under age 55 have been rising since the mid-2000s, showing the need for continued attention to awareness and screening.5
Unlike many other cancers, colorectal cancer is often considered highly preventable. Screening is the most effective way to look for signs of disease before symptoms appear and help find precancerous polyps before they develop into cancer. It can also detect colorectal cancer at an earlier stage, when treatment is more likely to be effective.7 This is especially important because a polyp can remain in the colon or rectum for 10 to 15 years before it forms a malignant tumor, and early colorectal cancer may not cause symptoms.7,8 For that reason, regular screening is important even for people who feel well and do not notice any warning signs.
The U.S. Preventive Services Task Force (UPSTF) and the U.S. Centers for Disease Control and Prevention (CDC) recommend that adults begin regular colorectal cancer screening at age 45. Screening is recommended through age 75 for most adults, while decisions about screening between ages 76 and 85 should be made on an individual basis in consultation with a healthcare provider, considering a person’s overall health conditions, prior screening history, and personal preferences.6,7
Some people may need to begin colorectal cancer screening before age 45 or be screened more frequently. This may apply to those with inflammatory bowel disease, inherited conditions such as Lynch syndrome or familial adenomatous polyposis (FAP), or a family or personal history of colorectal cancer or colorectal polyps.6,8 In these cases, screening decisions should be guided by a healthcare provider.
Colorectal cancer screening generally falls into two main categories: stool-based tests and direct visualization tests.
Stool-based tests are non-invasive options that can be done at home. Stool-based screening options include the guaiac-based fecal occult blood test (guaiac test), the fecal immunochemical test (FIT), and the stool DNA test.6 These tests check for signs of cancer or precancerous changes by analyzing stool samples for occult (hidden) blood or abnormal DNA.1 They're convenient, require little to no preparation, and offer privacy. Stool-based tests should be repeated more often than direct visualization tests.6
Direct visualization tests allow healthcare providers to look directly at the inside of the colon and rectum.9 These screening methods are performed in a clinical setting and can help identify polyps or other abnormal changes. Direct visualization tests include colonoscopy, computed tomographic (CT) colonography, and sigmoidoscopy.1
With several colorectal cancer screening options available, the fecal immunochemical test (FIT) can be a helpful option for people who may be less likely to complete screening when the process feels invasive, costly, and time-consuming.
As a simple at-home or in-office option, it offers a non-invasive approach that can help make screening feel more manageable. The FIT test works by using antibodies to detect only intact human hemoglobin and does not detect non-human and digested hemoglobin in the stool sample. As a result, dietary restrictions are not required before testing.10 When FIT is used as the primary screening method, it is generally recommended once a year.11
By reducing some of the preparation and inconvenience associated with some of the other screening methods, the FIT test can help make regular screening more accessible for certain patients. If a FIT result is positive, a follow-up colonoscopy is typically needed to complete the screening process.6
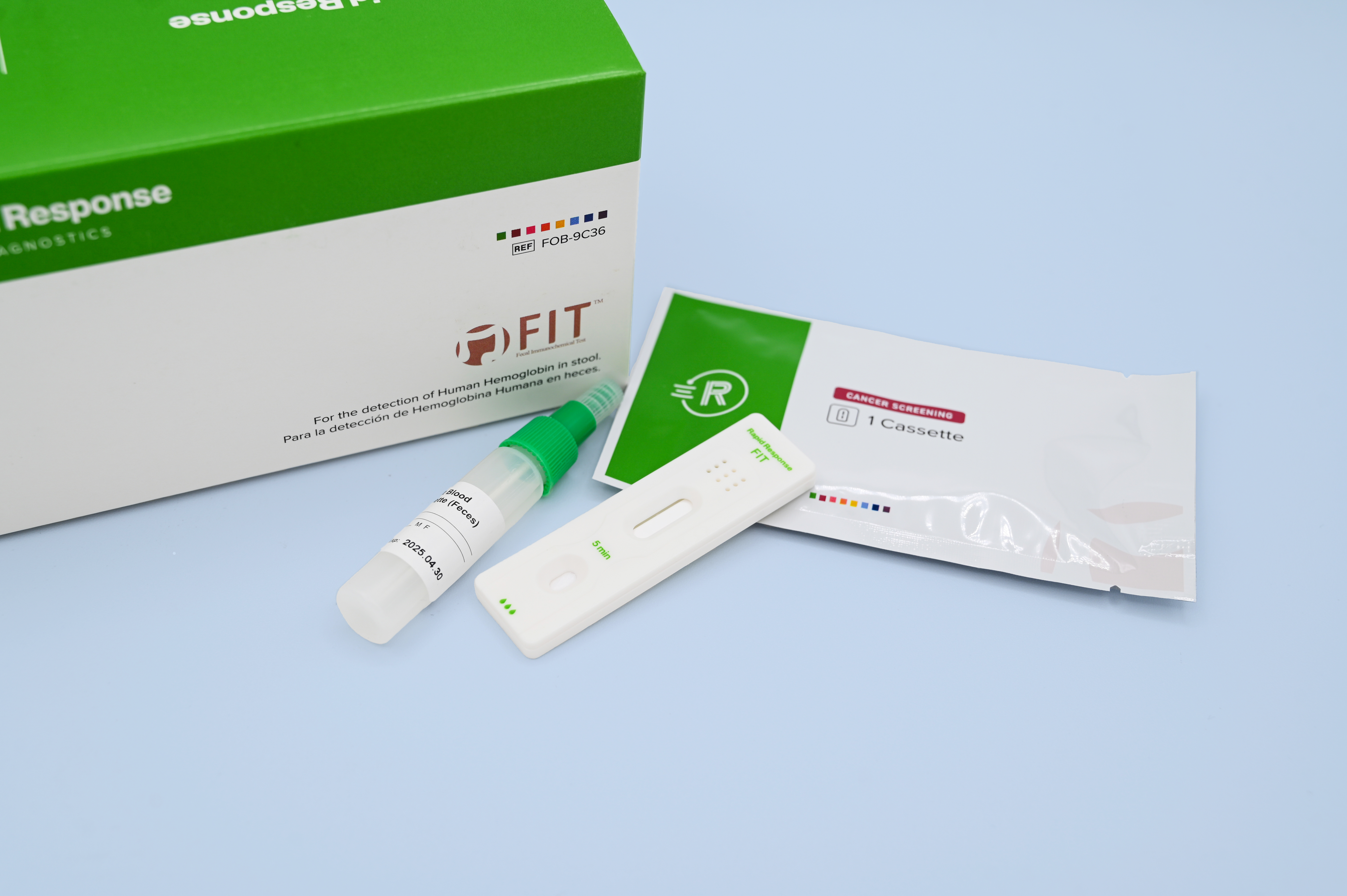
Rapid Response™ Fecal Immunochemical Test provides a simple and efficient solution for detecting human occult blood in fecal specimens.
This FIT test is designed to support family practice settings by offering flexible approach to colorectal cancer screening. It can be performed in the office during patient visits or offered as a take home OTC option, making it easier to incorporate screening into preventive health care delivery. This flexibility can help family physicians offer screening in a way that supports both patient access and practice efficiency.
- Detects hemoglobin in feces at a concentration of 50 ng/mL or greater
- Sample can be stored up to 24 hours at room temperature or up to 72 hours in a refrigerator
- No dietary or medical restrictions prior to testing
- Delivers results in 5 minutes
- Does not require specialized equipment
- Prevents unnecessary procedures from being done
With this FIT test solution from Rapid Response™, healthcare providers and organizations can support colorectal cancer screening programs in a more convenient and accessible way. Order Now.
- National Cancer Institute. (n.d.). Screening Tests to Detect Colorectal Cancer and Polyps. https://www.cancer.gov/types/colorectal/screening-fact-sheet
- Centers for Disease Control and Prevention. (2024, June 12). Colorectal cancer basics. https://www.cdc.gov/colorectal-cancer/about/index.html
- National Cancer Institute. (2025, May 2). Colorectal cancer screening (PDQ®)–patient version. https://www.cancer.gov/types/colorectal/patient/colorectal-screening-pdq
- Surveillance, Epidemiology, and End Results (SEER) Program. (n.d.). Common cancer sites—Cancer stat facts. https://seer.cancer.gov/statfacts/html/common.html#comparison
- American Cancer Society. (2026, January 14). Key Statistics for Colorectal Cancer. https://www.cancer.org/cancer/types/colon-rectal-cancer/about/key-statistics.html
- Centers for Disease Control and Prevention. (2025, February 26). Screening for colorectal cancer. https://www.cdc.gov/colorectal-cancer/screening/index.html
- Cleveland Clinic. (2025, October 28). Colon cancer (colorectal cancer). https://my.clevelandclinic.org/health/diseases/14501-colorectal-colon-cancer
- Hossain, M. S., Karuniawati, H., Jairoun, A. A., Urbi, Z., Ooi, J., John, A., Lim, Y. C., Kibria, K. M. K., Mohiuddin, A. K. M., Ming, L. C., Goh, K. W., & Hadi, M. A. (2022). Colorectal Cancer: A Review of Carcinogenesis, Global Epidemiology, Current Challenges, Risk Factors, Preventive and Treatment Strategies. Cancers, 14(7), 1732. https://doi.org/10.3390/cancers14071732
- American Cancer Society. (2025, October 15). Colorectal cancer screening tests. https://www.cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging/screening-tests-used.html
- Roshandel, G., Ghasemi-Kebria, F., & Malekzadeh, R. (2024). Colorectal Cancer: Epidemiology, Risk Factors, and Prevention. Cancers, 16(8), 1530. https://doi.org/10.3390/cancers16081530
- Qaseem, A., Harrod, C. S., Crandall, C. J., Wilt, T. J., Clinical Guidelines Committee of the American College of Physicians, Balk, E. M., Cooney, T. G., Cross, J. T., Jr, Fitterman, N., Maroto, M., Obley, A. J., Tice, J., Tufte, J. E., Shamliyan, T., & Yost, J. (2023). Screening for Colorectal Cancer in Asymptomatic Average-Risk Adults: A Guidance Statement From the American College of Physicians (Version 2). Annals of internal medicine, 176(8), 1092–1100. https://doi.org/10.7326/M23-0779
